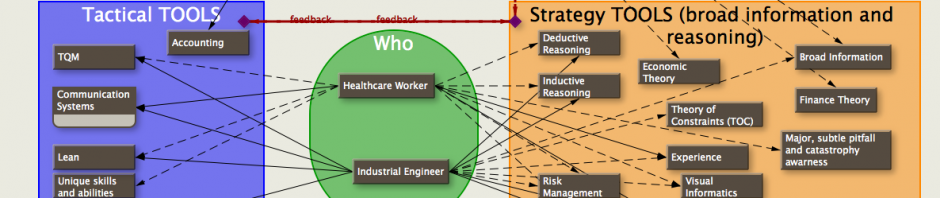
Can engineers and physicians mix?
When doing and hearing about healthcare performance improvement it seems much is dependent on doctors and engineers collaborating. Yet this is difficult. Sometimes impossible when implementing. Are they too different to succeed?
Juan D. Robles, Thomas Salerno and 1 other like this
30 comments • Jump to most recent comments
Wayne Fischer • [Hello, David! 🙂 ]
I’ve worked as an engineer in industry for 28 years and now in healthcare for 13. My work has taken me into just about every area of both. I have found no significant differences working with professionals in either domain. Most people are relatively easy and straightforward to work with; some are exceptions (for various reasons and with various idiosyncrasies), but I can’t say MDs, as a group, are much different from PhDs in industry. 🙂
Brian Gregory, MD, MBA • Not a problem.
David Belson • The reason I wrote this is a very large healthcare organization asked why doctors seem to be a roadblock in sustaining change and systems redesign. They felt that the approach of engineers is quite different from doctors and full implementation of engineered improvements is often a problem.
Not sure I’d hold up PhDs as a good example – and I am one.
After over 40 years in industry, last 12 exclusively in healthcare I believe that doctors present a real challenge. Their approach is quite different. Doctors diagnose and engineers design.
Not sure how to answer the question as to how to maximize the effectiveness of the combination.
Brian Gregory, MD, MBA • “Doctors diagnose and engineers design.”
Um… You’re kidding, aren’t you? Stereotyping? You are aware that many physicians are also engineers, PhDs, etc.? Diagnosis is also integral to good engineering.
I suspect that the problem lies in what’s in it for the stakeholders. An engineer gets paid to change the system. Change can cost time and money for some physicians. Who’s paying the engineer to change what for whom?
Bureaucrats love bureaucracy. Lawyers love going to court. Surgeons love cutting on people. Citizens, defendants, and patients aren’t as fond of those events.
[Pardon my stereotyping for that last sentence, but the not totally accurate stereotyping was a quick way to emphasize the point—and in this case helps, not hinders, the thought process.]
Brian Gregory, MD, MBA • There’s also a lot of ‘systems engineering’ that physicians design, create, and employ throughout healthcare with their procedures. (spoiler alert: the human body is a complicated system, too). It’s just not the type of systems engineering that you’re familiar with.
Wayne Fischer • Brian beat me to the punch – I agree with all he wrote.
I also heard from others early on in healthcare that physicians (and especially surgeons) were “hard to work with.” I never found that to be the case. I think Brian’s got it right: finding out what the physicians’ need to do their work better, faster, cheaper, easier… 🙂
David Belson • Sure, sometimes MDs are part of management engineering. Some are great to collaborate with. I just published a paper with one.
Question is how to assure physician support and involvement? This is not always the case. What creates MD-Engineering success?
Medical schools don’t often include training in systems redesign or such things as Lean. I have been working with a medical school but they find it difficult to include it in their busy and expensive curriculum.
Brian Gregory, MD, MBA • David, I will agree with you some specialties need to broaden their focus. 17 years ago, whilst as KFSH&RC, I was chatting with an visiting anesthesia attending (professor) from some name-brand school that they needed to include game theory in training for anesthesia. He didn’t know what I meant.
I tried to explain in terms of risk management, constraints, efficiency, drug dose and fluid challenges during a case, and playing chess—he still didn’t understand even after I gave some examples from routine cases and a couple of trauma cases. Clueless still– his eyes crossed with boredom from listening to me. The topic was also a non-starter at a couple of M&Ms.
But, I’ve had some good conversations with non-teaching anesthesiologists, pulmonologists, a nephrologist, some cardiologists, a pediatric surgeon, some OB-Gyns, an ER doc, and a couple of others about the same topic. What does that mean? To me it means that some people and specialty programs are a lot better than others.
Systems engineers are not a homogenous bunch either. If either physician or engineer is out to lunch, there’s not much synergy.
But—As Wayne said…”finding out what the physicians’ need to do their work better, faster, cheaper, easier”…is very important and often overlooked while the engineers try to force implementation of something that adds no value (and sometimes decreases value) to physicians.
Med school is not the right place for training in lean management. Residency programs would benefit more from game theory, risk management, constraint theory, sequencing analysis, and a bit more statistics and probability focused on their specialty. Lean is common sense after all those.
Wayne Fischer • From what I read, and have heard, more medical schools are including aspects of Quality Improvement in their curriculum. IHI has instituted their Open School Quality Improvement Practicum, and there are plenty of other resources (on-line and elsewhere) for docs to (self)learn QI.
When working with docs I don’t mention the catch-phrases (Lean, Six Sigma, Theory of Constraints, etc.) but rather engage them in a dialogue from which I try to learn what it is that they need…in their context…their world, then propose an approach I think will work, explaining as I go (when needed) what and why the different methods / data are that we’ll use.
But generally, isn’t your main question of “how to assure physician support and involvement” answered by the tried and proven concepts / principles / methods of change management? [Well, they’ve worked for me…]
Brian Gregory, MD, MBA • Always a pleasure, Wayne. 🙂
Arie Versluis • Wayne and Brian did give already some very good comments – I had not expected otherwise.
In my experience as an industrial engineer (with a strong behavorial science background) I never had any problem working with the medical profession, not even in University hospitals :-). My approach is to show doctors – and others – that I understand their profession and its organizational issues that come with that and by talking with them (not to them) I can let them develop a feeling for my profession. From that point on we can cooperate as professionals in improving the service to the patient.
The discussions about doctors against engineers is mainly found in hospitals where the engineers (often supported or pushed by management) think that they are the only ones who know how to design good processes and a good organization. And then try to impose that on the professionals and other staff.
David Belson • Thanks for the comments. We were seeking ideas to improve the collaboration. I am
sure there are many success stories.
There are differences between their training and viewpoints. Doctors often focus on the individual and relating to the individual’s problems. Engineeres, I believe, are more systems oriented and rely less on relating to individuals.
As Arie said; imposing engineering designs on doctors is doomed.
Richard Skiff • This is a very interesting discussion. One thing that helps when approaching a problem (something that is different than what it should be) is to mutually define the problem, and to focus on how that problem can be solved – from the perspective of value to the customer. This also requires a discussion as to who the customer really is. In some cases it is the patient, others the physician, others the “system;” and often there are multiple customers. Once we have a mutual understanding (hopefully agreement), then working on countermeasures to the problem becomes a collaborative, rather than a confrontational, endeavor.
Brian Gregory, MD, MBA • David, I believe that you have a preconceived notion that you won’t relinquish.
David Belson • Richard: Good point. I’d pose the problem as – how to you improve (or assure) a productive relationship between doctors and engineers, particularly sustaining change?
Brian: This was not my idea, was asked this by a very large healthcare system; a “customer” who invests a great deal in systems reengineering but feels doctors do not always support the designs in the long term.
Madhan Kris Srinivasan • Richard and David: Great discussion points! As a systems engineer and physician, my take is to work back from a common goal. Many times in healthcare, we are so consumed with the immediate problem that we lose sight of our end goal, which is usually good patient outcomes. In my experience with medicine and risk management, I utilize this basic concept to make even the most complex processes simple. It has and still is working for me.
Brian: You raise many good points, but one that I will argue is that lean management should not be taught in medical school. This is where the foundation of every physician is built and if we do not instill some insight into such thinking at this stage, the future is uncertain. Systems thinking can benefit a student even in their daily activities while trying to complete multiple given tasks. I agree that game theory and predictive modeling too over the top, but the basic concepts should be ingrained at an early stage.
Group: Systems thinking needs to integrate with the physicians behaviors while not affecting our autonomy in decision making. If this happens, then engineers are viewed as no better than payers who are controlling decisions whether they are in the best interest of a patient. So the goal of all engineers should be to integrate their thought processes where it fits into that of any physician. My suggestion would be to have systems engineers shadow physicians for a given time and get a true sense of the behaviors, stressors, and optimal practices currently being used but not shared.
Brian Gregory, MD, MBA • The point of my recommending teaching systems engineering skills in residency is that the benefits of the techniques will be obvious and appreciated each day. The residents will accept it as readily as the learned clinical techniques for a patient. Residency (not med school) is when you begin to see the business side of medicine. It will also increase the throughput in each specialty (which is often a problem with residency programs) in the hospital. The focus, feedback, and social pressure just isn’t there in med school (IMHO).
I’ve worked with groups of neurosurgeons who trained at different facilities. One group was from Tennessee, and you could tell that their training included ‘lean’, contraints, strategy, and teamwork. The other group was more of a circus act.
I’ve also noticed considerable difference in new anesthesia group members. Some hit the ground running, others seem to be road kill for the first year or two. You can tell who has had some systems training (whether it was formal or informal).
Robert Gordon • I wrote a long note about the different place and perception of “physicians” and “engineers” in healthcare. But the length was all cleverness and learning. Cut.
Forget the labels. People with the ability to see systems and an interest in re-designing processes, whatever their titles can make valuable contributions. People called “doctors” (can) know process and “engineers” (can) know healthcare.
I have met conceited, arrogant, jerks bearing each of those titles. The people who were the opposite of that (open, participative, gents) were the way they were by character or personality, not by undergraduate degree.
The way this thread was introduced (however well intentioned) risks exacerbating any lingering status worries and making progress more difficult rather than less.
Brian Gregory, MD, MBA • “Brian: This was not my idea, was asked this by a very large healthcare system; a “customer” who invests a great deal in systems reengineering but feels doctors do not always support the designs in the long term.”
David,
Taking a cue from Robert’s comment, if you’re interested in helping your ‘very large healthcare system customer’, I’d recommend suggesting they hire some physician-engineers with a good theoretical background and practical experience to act as translators and evaluators of those systems. They’ll be more apt to find the ‘systems engineers’ on the medical staff and bring them on board. They’ll be more able to help clarify the needs and tailor those systems directly and indirectly by putting the right people together with the official systems engineers. Find and give the embedded natural process talent some power.
Heads of departments aren’t necessarily the ones with the background, savvy, and inclination to change things. There are probably other docs who have been thwarted in bringing change by the current political and hierarchical structure within the facility. Make it possible to bypass that structure.
Arie Versluis • Often when I read discussions like this one I have a feeling that one of the implicit assumptions is that there must be a best solution for organizational and process issues. Solutions which, when found. can be applied in the whole organization.
I have learned from my experience – I learn from my mistakes 🙂 – that these implicit assumptions are the cause of a lot of frictions. And what is the best solution today maybe completely obsolete tomorrow because the healthcare world is very dynamic and has strong stochastic characteristics.
@David: I have found that collaboration can be realised very well by implementing multidisciplinairy teams and give them on the operational level the authority and responsibility to design and implement their best processes (with a little bit of engineering help). The structure and activities of these units are based on applying ‘minimal specification’ for the design, instead or the traditional maximizing of specifications for better control. By allowing decision making on the operational level flexibity of those units is very high. And yes, it can lead to situations where to comparable units choose different solutions. And I think that is great! Those units can even learn from each other.
Lynne Sisak • David and Brian – I agree with you both almost fully! I am not a physician nor an engineer but usually the person who brings these two parties together. Both respond well to data – I’m talking real data here. What I have seen is that physicians tend to see the black and white of things while engineers see the grey in between. The other characteristic that I see is that physicians (and yes, I am generalizing) tend to make decisions quickly where as engineers need to ‘think’ about it for a bit before making decisions. If the goal is clearly stated at the beginning and both parties can articulate the goal to each other – puts everyone on the same page – and a third party (the role I play) collects and presents the data to open up the dialogue – works like the charm. I respect and truly enjoy working with both – but they are very different.
Brian Gregory, MD, MBA • Lynne,
Your talking to an anesthesiologist here. We work in shades of gray:
Never trust a single monitor or piece of equipment, all patients react somewhat differently to drugs, batches of drugs have been known to fail, type of anesthesia can depend on the surgeon as much as the patient, trial and test are sometimes the only way to know what will work. It’s a fuzzy world and we feel our way through it. Gotta have a backup for everything. But you still need to know the theory to work your way through the fog.
Brian Gregory, MD, MBA • Did I mention that sometimes the theories conflict?
Lynne Sisak • Brian – I agree with the process for decision-making … yes, you take all of the variables and make a decision – I don’t consider that exactly “grey”. What I am referring to usually occurs after that. So once a decision is made – it’s fairly final from an MD point of view. To the engineer it is never final. And just so we are clear …. I’m not suggesting that MDs can’t change their minds and make a different decision later, it’s just that to the engineer, the decision was never truly final in the first place. Just my observations …. been in the business since 1979.
Craig Dreikosen • I have gotten along wonderfully with our Physicians. Contrary to some of the comments in this post I feel Engineers and Physicians actually think, act, and are trained in very SIMILAR ways. Engineers are problems solvers…they look for solutions or at least a partial solution to everything. Physicians do the same with the most complex organism (system) that we know, the human body. In my mind you can actually lump the two of us into very similar pools and I find the synergies are amazing.
Brian Gregory, MD, MBA • Lynn,
Hmmm…’fuzzy, fog, trial, test, conflicting theories’— Those don’t sound like inflexible decision adjectives to me. If you’re using “grey” to mean that you don’t really know what you’re doing or what you should be doing, are you applying that adjective to engineers? Lack of detailed feedback can make it difficult.
I’m confused…been in the business since 1978.
Brian Gregory, MD, MBA • Lynne, you said: “I am not a physician nor an engineer but usually the person who brings these two parties together.”
How do you do that? Bring the two parties together? Do you have an analytical mind and detailed information or resources of another sort (financial analysis, financial backer, legal, rules and regulations, contacts) that those two parties need to work synergistically? Are those two parties within the same facility or across the country? Are you more like an angel or a dating service? Is this necessary extra component of the physician-engineer mix unique to your facility, company, or situation?
What’s your value added?
Douglas Zech • All,
Very interesting exchange, for which I thank all the contributors.
I have had similar experiences to the one David puts forth in the question. The first reaction for many is “Docs and Engineers can’t play nice together” but I think that’s too simplistic. My take is a “5 whys?” exercise is needed to figure out where the issue really lies. I’ve found external physician groups often have much different goals than the hospital, so they’re not really working towards the same endpoint as the hospital engineers. (I don’t have much experience with employed Physician groups, so maybe it’s not an issue in those hospitals). These goals have lead to conflict at the process level between the Physicians and the Process Engineers. These are separate issues which evolve at the Sr. Management level, but the Engineers and Physicians are left to battle it out far removed from the ivory towers. It seems I’m often working with a Physician who’s playing Baseball, while I’m standing there holding a football!
I’m going to try to be nicer to those darned Physicians going forward!
Lynne Sisak • @ Brian – yes – except for the dating service part. And typically within the same organization.
@ Graig – If Physician and Engineers were the same then we wouldn’t have one or the other. I am not favouring one over the other – I’m just saying they don’t think or problem solve the same way – generally speaking of course. If they did, then all Engineers would have gone to Medical School and all Physicians would have gone into Engineering. But they didn’t.
Brian Gregory, MD, MBA • ::grin:: Thanks, Lynne. I marvel at your logic.