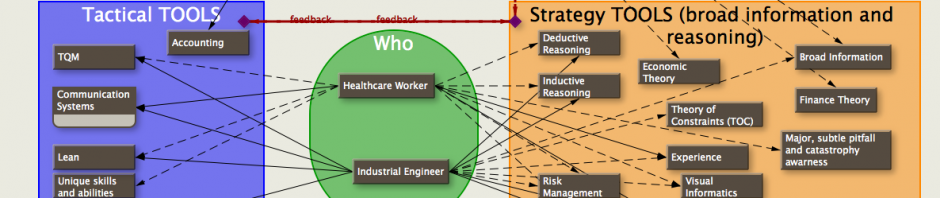
The following are excerpts from a discussion concerning Turn-Around-Time (TOT) in the OR. They relate to my recent posts on scheduling, and show the complexity/difficulty in defining the problems and solving them:
____
she:
There are benchmarks out in the industry, Advisory Board and OR Manager are two that compare procedures and organizations. The definitions for turn around time are different depending on whom you are talking to. Wheels in to wheels out is used by many facilities and staff. The surgeons consider downtime (close to cut) as the turn around time.
There are many factors which impact turn around time and it can be a complex to address. I would be interested in your experience with aligning the expectations of the identified groups.
_____
me:
The turnaround time can adjusted to whatever you want, even a negative time. It just depends on how you define benchmarks, and what resources you want to throw at it. The trick is to not make the other resources angry when you’re focusing on appeasing a particular subgroup of people.
As for benchmarks:
The benchmarks just tell you what other facilities have done, and may be a terrible goal. There’s been a long discussion on the hme sites about the meaning of benchmarks, and the consensus is that it should not be a goal. In fact, a particular benchmark might make no sense at all in your situation.
_____
she:
I agree with your comments on benchmarks. It is difficult to compare apples to apples with so many variables between hospitals. However the clients I work with ask for various benchmarks. I prefer to look at the current state, where the opportunities are to improve and work on practices that have had an impact on TOT.
______
me:
Sounds good. If we define the question well enough, the answer becomes a bit simpler. I’ve put together a model that takes into account most of the common factors that affect TOT (and can easily throw in those weird, idiosyncratic factors in particular facilities) and can give you TOT to the minute depending on what you want or need to adjust. I suppose the most valuable part of the model is that it keeps you from wasting resources on improving factors that have only minimal or no effect on the TOT that you define. So, if you define a little further what they’ll let you alter, and what’s a sacred cow, you can come up with the different costs in time and money for the different agents (hospital, anesthesiologist, surgeon) involved. You tell me what you can change…and I can tell you in detail what you need to change. How you change it will involve varying amounts of money, politics, and patience. And, ideally, you’ll have some bright person in charge at the appropriate operational level who will say “Yeah…I can do that!”