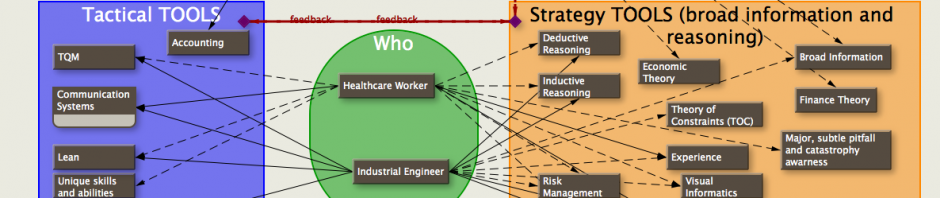
Is Healthcare’s Insular Culture a Liability or Benefit?
Working recently in the healthcare industry, I keep being struck by the deep-seated culture that unless the solution or practitioner is from healthcare, then it cannot be applied to a solve a current problem. Due to the importance of many solutions in terms of human life, I can understand this perspective. But, it seems to exclude perfectly viable options that work successfully in other industries. I am wondering whether this mindset is becoming a liability to implement changes in teh industry? Or is it good and “healthy”? I would appreciate any thoughts.
- 4 comments
Lewis Hooper • Peter,
Sorry for the late response to this. I think your point actually scratches a couple of deeper points. I think the “do no harm” philosophy of patient care does dictate some resistance to change, but I have come to believe there are other important factors at play. Some of these are:
1) The inherent structural leadership problems in the way we organize much of healthcare (especially Hospitals) where professionals may have different agendas than the corporate agenda. The result of this is that go forward consensus is very difficult to achieve.
2) A funding/political governance system that frequently punishes innovation. Innovations that close beds are political death for the CEO, and in a fixed global budget environment innovations that improve throughput of inpatients drives cost beyond revenue resulting in financial difficulties.
3) The lack of a clear motivating force for the corporate end of the organization. Business can fall back to its financial motivation, make money, this is clear and simple. Healthcare is not as simple. The driver of providing good patient care founders quickly on which patients at what cost, and sometimes on whose patients (see #1 above).
I am sure other readers could refine this list and lengthen it a great deal, but they all lead to a skepticism of any idea “not invented here”
One way around these barriers may be to work closer with the front lines. Healthcare is a pretty dynamic environment at the front line. The treatments and methods used to care for patients seems to change faster than the structures we put in place to organize and assist care. If front line folks can be convinced of a tangible value for their patients, they seem to make things happen.
Bottom line is that I agree that the “mindset is a liability” but it’s not just cultural, there are significant structural issues. There may be contingent of folks who are willing to look outside the box, but its a hard sell.
Interesting observation, thanks for having the courage to post it.
Robert Gordon • Good response from Lewis. VERY important “other important factors”!
But the general “do no harm” value structure does need to be explored a bit more than that to address Peter’s open and honest question, with an apparent admission of newness to the “industry”. [local terms: Practitioner = Provider = Professional]
The “do no harm” value is not only an internal ethical motivator of the caring professions. It is also expressed in criminal laws as well as in ministerial regulations and in the standards of the Colleges that govern “healthcare disciplines”. It is also the basis for calculating malpractice insurance, both in premiums and in the adjudication of claims. [Note that managers and consultants who propose changes pay no such premiums because they face no such risks.]
I do not believe that providers resist the expertise of “outsiders” as such. I have seen providers listen with docility or at least respect to physicists, statisticians, geographers, classical scholars, self-made tycoons, etc. However, an “outsider” is by definition someone who does not know what goes on “inside”. This should imply that outsiders will be receptive and humble about their own thinking. Alas, some outsiders approach their efforts to make a difference in healthcare (which is often given the title of “most complex activity on earth”) as though they know more about it all than those who are insiders. Such an approach will instantly reduce the credibility of such an outsider and probably make it harder to open ears even to simple explanations and facts.
Although it is as true as a truism, it is often judged tedious to say that “healthcare processes are unique”. OK. Let it be said that “Lean manufacturing processes are unique.” To deny that would be to say that Ford and Ohno et al. discovered nothing. So now, calm down, and accept that healthcare processes may be different from those imagined within TPS, SS, and Lean. [In fact, stereotypical healthcare processes are in certain respects, of more or less significance, essentially different from those of manufacturing.] But how (where) are they different? How (where) the same?
The most common cause for healthcare providers’ resistance to adopting operational change(s) in their work is that they are not convinced that the change will provide a net benefit to anyone involved (except, cynically, careerist managers, consultants, politicians, etc.). Who has the onus to convince them? I would say that the onus is on the proposer, even if (the proposer honestly believes) that the change would in fact be beneficial to patients (in whatever “term frame”). So what can the proposer be reasonably expected to do to convince providers?
1. Demonstrate full understanding of the current healthcare processes.
2. Understand that proposed changes are improvements to existing excellence.
3. Listen to objections as though they were valid
(they probably are).
4. Listen to providers when designing the implementation plan
(they know where the dragons’ dens are).
5. Don’t start implementing until you have a plan that will execute flawlessly.
The Lean Value Law applies to process improvement processes too:
“The activity must be done right the first time.”
If you cut the wrong vessel, the patient will die.
If you administer the wrong medication, the patient will die.
If you give the wrong exercise, the patient will die.
Brian Gregory, MD, MBA • With your question, are you differentiating between the healthcare administrator and the clinician?
Many clinicians understand and practice efficient, safe, productive techniques. Many non-clinician healthcare administrators do not understand ‘good’ operations management processes, nor how to integrate them into clinical practice.
Here’s a study by Amanda Goodall, “Physician-Leaders and Hospital Performance: Is There an Association?” It begs the question as to the benefit of corporations taking over healthcare. Is the question of culture one of ‘clinical’ culture, or ‘hospital administrator’ culture?
http://ftp.iza.org/dp5830.pdf (graph on page 18 for gist of article)
Personally, I’ve seem many a physician cringe (due to inefficiencies and wasted time) whenever they had to take a case to the hospital instead of handling it at their own surgery center.
I’ve close friends who have worked daily with C-level administrators, processes, and programs in many hospitals to troubleshoot problems. I’m constantly amazed by the following of the latest fads, the lack of an holistic understanding of processes, and the lack of leadership as evidenced by the stories I hear.
Is it the clinicians? Or is it the current MHA ‘culture’ running the show that inhibits progress?
Peter Hadas • Thank you, fantastic insights. In some ways it answers my question, in others it begs more.
Lewis, I am curious about your comment on structural leadership problems driving different agendas. I have done executive leadership alignment and strategic planning work and competing agendas are the norm, regardless of industry, company, etc. Is this comment related to hospitals having multiple ‘power-brokers’ (e.g., operational administration, clinical leadership, legal/privacy) rather than a more typical hierarchy that exists in some form, however matrixed, in the private sector? Or are you refering to other structural issues?
Robert, I fully agree that some ‘experts’ waltz in with their brilliant ideas and try to impose their genius upon others without first trying to understand the people they are trying to ‘help’. As Stephen Covey said, “Seek first to understand, then to be understood”, and many of these individuals do this in the reverse order, and then stop half-way. What gets me though is this filtering that seems to happen right up front. And the filter is whether you have the right credentials, and the credentials are whether you have worked in healthcare. Now I am fortunate in that I have worked in healthcare and life sciences off and on from the very beginning, so I seem to be accepted long enough for people to actually allow me to ask questions in order to understand them and their situation. However, I continue to be surprized by that initial mindset that sends the message, “unless you’re one of us, we’re not prepared to listen”. I know it sounds drastic the way I have worded it here for impact, but the general gist is real – I have discussed this with colleagues within and without the industry. And I am just wondering whether that cultural or mindset barrier is preventing the openess required to consider solutions that worked elsewhere to see whether they could be adapted to healthcare realities?
Brian, interesting distinction. Here in Canada, the trend mentioned by Amanda Goodall, seems to be going in the other direction. At least here in Ontario more clinicians are entering the administrative ranks, which seems opposite to what is happening in the US and the UK. The most visible difference, at least publicly, is that patient-centred care is rising in terms of importance and is now competing with cost and financial considerations. Still, I have not noticed a difference in that mindset with either administrative or clinical staff, but now that you have pointed out the difference, I am going to pay closer attention to see if there is a difference.