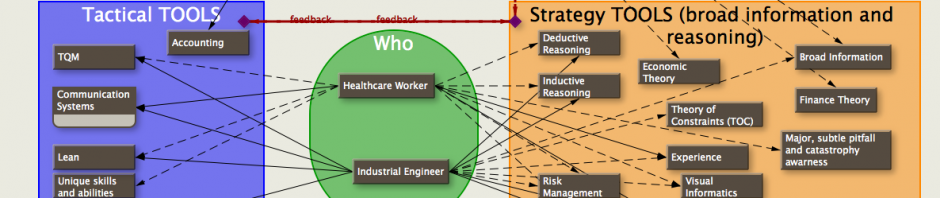
How will medical tourism insert itself into the mainstream of U.S. healthcare reform?
Under healthcare reform, employers are beginning to express interest in concepts and reform measures which have variously been labeled ―value-based, ―results-based, ―performance-based, or ―outcomes-based purchasing and bundled reimbursement for an episode of care. The bundled payment methodology that works well in medical tourism is challenging for most U.S. healthcare providers because legacy systems support and maintain “-silo-based”, and “-impression-based purchasing” and limited reporting capabilities, when you get right down to the core requirements for actionable insight.
While employers have access to new and innovative tools to pair sophisticated data integration technology from products such as Johns Hopkins Adjusted Clinical Groups® (ACG®) System with customized preventative care and employee wellness programs and convenient mHealth and easy-to-use applications such as the Lifestyle Risk Calculator® integrates evidence-based, health care delivery and cost avoidance by capturing all clinical transactions (including biometric monitoring of vitals for each employee and dependent). At MHI Benefits Group, we sell that capability to employers for as little as 5 cents per employee, per day.
The Johns Hopkins Adjusted Clinical Groups® (ACG®) System, and its competitors in the space, offer a unique approach to measuring morbidity that improves accuracy and fairness in evaluating local and regional provider performance, identifying plan particpants at high risk, forecasting healthcare utilization and setting more defensible payment rates. These are an integral part of value-based purchasing, because value-based purchasing initiatives aim to improve quality of care while avoiding unnecessary healthcare delivery and their associated risks and costs. While I can appreciate their “aim”, I am not so sure they hit many bullseyes.
One major concern in healthcare reform, not just in the USA, but all over the world, involves the significant variation in practice patterns observed both across and within regions, which prominent research has argued does not improve quality of care even though these patterns entail large differences in resource utilization.
Therefore, as I see it, the most difficult challenge for medical tourism to overcome, is to insert itself into the mainstream of health delivery reform choices. The choices will initially be made by super consumers (employers and insurers and other group health purchasers) and individual consumers (plan participants). But who will they choose? What and how will they measure and make comparisons? Where will the data come from and how will it be measured? How will the value be portrayed and presented? What will bring this choice to front-of-mind? As the CEO of the largest medical tourism network for group health, together with our authorized brokers and agents, we struggle with these answers for clients on these questions every day.
The power to change healthcare comes not from doctors or health plans. It comes from primary, reliable data that is informative and actionable. When the data is useful and credible, plan administrators, physicians and patients will all be enabled to make better treatment and lifestyle decisions. I invite you to share some solutions you may have identified along the way.
36 comments • Jump to most recent comments
Maria K Todd MHA PhD • To begin to solve this, the disparate data and coding nomenclature systems (internationally) and data silos associated with regional provider networks and TPA legacy systems (domestically) must be reconciled in order to integrate the data to measure an episode of care. I don’t see advances in functional interoperability to bring practicability to the marketplace. At MHI, we do this for our group health clients by hand. Ugh! It is complicated and takes specially trained analysts that no university health administration program is producing.
For example, complexity arises from the fact that a plan member using a medical tourism benefit may have care in three places: pre-op services/diagnostic testing in one location, surgery/some rehab and recup elsewhere, travel back home associated with potential complications such as DVT VTE/PE that could result in readmissions or death, and post-op follow up back home. This data must then be integrated into a system that was never designed to integrate an episode of care delivered in this fashion.
Next, the coding nomenclature brings baggage with it. Case in point: a surgical CPT code generally includes a follow up period of 10-90 days depending on the case, and the surgeon that performed the procedure is expected to cover that follow up at no additional charge. A surgical CPT “is” a bundled rate. What is necessary is to re-packaging it to redistribute the reimbursement and pay those who are involved in a medical tourism episode of care. But how will these tricked out new evidence-based medicine software packages evaluate a medical tourism episode of care? Will it throw a red flag on the play? on the physician? They didn’t do anything “wrong”. What is “wrong” are the business rules that supply the logic to the software.
While existing technology and software applications to perform population health management is readily available, when we work with clients to define a medical tourism benefit option, we encounter few employers that utilize all these great new tools for risk stratification. Some assume their TPA does it or disease managers use it to manage cases. That tells us that the plan administrator (PA) is not really “administering” what they could to mitigate risk, (a plan fiduciary implication under ERISA, but that’s a topic for another day). If readily available combinations of tools are not being used when they are available, then actionable steps are missed. Reports may be ignored, useless, unavailable, too confusing, overwhelming, or unreliable. Regardless, the result is “impression-based purchasing” instead of value-based purchasing.
We often carve out the entire medical tourism program for group health because the TPAs are often unprepared to handle bundled claims, cannot integrate reporting, foreign currency, or bundled provider settlement. Since we handle the logistics for the entire episode of care, we have access to all data to integrate it back into the system. For each case, this takes about 3 hours to perform manually. To do this, we have to override the rules engines and create custom reports, because the software logic is rules-based, and the rules are based on yesterday’s health delivery, not that which has been reformed to include medical tourism. Until the market demands that the analytics product “produce” the data to make better value-based purchasing decisions, it will continue to use its artificial intelligence to “think” and measure performance inside the box.
Meanwhile, medical tourism and other innovative cost saving and valuable solutions will likely remain outside the mainstream looking in, a tragic loss of cost avoidance and value-based purchasing opportunity for most of the nation’s 210,000 self-funded employee benefit plans and their plan participants.
Brian Gregory, MD, MBA • Maria,
Do you have any guesses as to what politics will come into play if a large portion of lucrative procedures start moving overseas? Doesn’t seem as though the medical lobby will like its business off-shored unless they have their hands in the pot. There are lots of possibilities as to how this could play out, and I don’t have a feel for the probabilites.
Maria K Todd MHA PhD • You know Brian, I hadn’t given that any thought. Probably because to me, whenever I hear about the medical lobbies from doctors, it is accompanied by a groan. I would guess perhaps they will need to consider auxiliary chapters offshore, rather than try to control the flow. Many docs that are considering the potential to offshore cases and travel with the patient (a form of concierge model care we are seeing more and more frequently) would gladly accompany a patient for surf, sun and surgery in the Caribbean or some other exotic place that allows them to stack cases with a temporary or provisional license or a local proctor arrangement.
I would guess the hospital administrators would be the first to wince, rather than the lobbies. Actually, it would be a viable alternative response to the moratorium on physician-owned hospitals. As you may recall, physician-owned hospitals, popular in the 1990s, sparked intense battles within the hospital industry for years. The facilities’ rivals — non-profit community hospitals and for-profit institutions without physician investors — were able to motivate Congress to pass a lengthy moratorium on the construction of new doctor-owned hospitals that specialize in cardiac, orthopedics and other specific areas back in 2003.
The new law is much tougher. It applies to all physician hospitals, even those that aren’t specialty facilities. Besides barring new doctor-owned hospitals after this year, it prohibits the 269 existing institutions from expanding unless they meet stringent conditions. As a result, backers of the physician hospitals say, the new law is something of a legal minefield for doctors’ facilities. But, not if they offshore, outside the scope of the moratorium. If not repealed, I could see a strategy play by members of Physician Hospitals of America, a trade group for doctor-owned institutions to get behind this alternate venue movement.
However, given the nature of these procedures, the volumes are somewhat limited by trauma cases that I guess could be stabilized and then transported to some other destination by an agency such as OneCall (hey Phillip are ya listening?), those cases limited by co-morbidity and concurrent conditions that restrict travel, funding sources (Medi/Medi), or cases not accepted by the receiver destination for whatever reason. So, I don’t think they will be “significant”…at least not for a few years’ time.
Brian Gregory, MD, MBA • Hmmm…disaster and opportunity all rolled into one. Lots of ramifications from your information. Think I’ll short some selected hospital stock on Monday, and check out practice opportunities off-shore on Tuesday
Scott Frankum, MBA • Hi Maria,
You pose a big question, but maybe these two notes will help. The Health Information Technology for Economic and Clinical Health, (HITECH) act passed in 2009 as part of recovery legislation. This law provides the technical foundation for meaningful measurement and interoperability of health care data. It is a real, tech backbone at the 7th level (I think) trunk, so it can be private. It is not functional yet, but will be soon and I understand it will deal with the problems you surfaced together with new services like mHealth and cloud capabilities.
Traditionally, the health care industry is not standardized between or among stakeholders. So, standardization of health data capabilities is a planning-heavy effort. The ACA’s administrative simplification to standardize data entry is another big piece of the transformation to universal measurement.
Your question about reform inputs seems to be from the provider side. My understanding is that bonus payments and ratings will all be from the customer results side. For example, ACOs take 36 patient quality measures like blood pressure, weight and lab data together with measures like hospital re-admissions to determine reimbursement rates. So…the relevant data will be mostly real patient data or objective observation.
The ACA is largely, the story of building the capacity to measure quality, throughout the entire health care system. Measuring quality is entirely new to U. S. health care and is key to driving consumer value.
Michael Porter captured the priorities to quantify medical treatment quality by defining value as medical outcomes per dollar spent, (value = measurement of outcomes ÷ money spent). We’ll measure everything, so health care quality can finally be managed throughout the entire health care system.
I can’t find it in any literature on reform, but Drs. Porter and Teisberg confirmed this foundational equation in an email to me.
The numerator will include medical quality, defined as: high patient medical outcomes, seamless care coordination, high customer satisfaction and payment methods that are not linked to the volume of care delivered.
Brian Gregory, MD, MBA • Scott,
IMHO standardization of healthcare in the US at this moment in time would inhibit real progress.
Accounting and finance in healthcare needs significant work (I’ve academic friends working on that); preventative medicine (diet, exercise, screening tests) need to be integrated; relevant, actionable data based on proven theories and experience need to be collected (my OR experience convinces me that’s decades away), and people with strong backgrounds in several disciplines need to coordinating this (those people are not yet in positions of power in significant number).
Standardization should be a means of collecting data to improve care, but I’m leary of it being a hindrance to innovative (for healthcare) changes.
Scott Frankum, MBA • Brian,
I totally get the point that innovation is messy. Just to clarify, reform does not standardize treatment….it only standardizes the measures of results and reporting…which should regularize accounting / finance too.
Maria K Todd MHA PhD • Scott,
“The numerator will include medical quality, defined as: high patient medical outcomes, seamless care coordination, high customer satisfaction and payment methods that are not linked to the volume of care delivered.”
Would you disagree that the volume of cases can directly correlate to the quality, outcomes, seamless nature, and high customer satisfaction? Is this volume upon which Centers of Excellence are essentially based?
Having a problem with, I am “the volume of care delivered not linked”, young Jedi.
Brian Gregory, MD, MBA • Scott,
Agreed. You need to standardize reporting to make improvements. But with experience and greater understanding, those ‘standardized’ reports should evolve. In systemskk engineering there’s a saying – “Show me what you measure and I’ll show you what people will do.”
Guess I’m saying that care needs to be taken to not solidify a standard if it can still be improved through better understanding and morphing. Tough job to do it well.
I suspect that some progressive facilities would be creating their own ‘improved’ reports in parallel.
Scott Frankum, MBA • Apologies for that. Let me de-code. You kind of covered the topic in bundled payments.
I know this won’t be news to you, but may be helpful for others interested in ACA issues.
From Volume to Value
Fee-for-service medicine means that you are charged a separate cost for every single service and cotton ball used in your care. If you have ever gotten a confusing, multi-page invoice for a medical procedure, fee-for-service medicine is why. Reform seeks to shift payments for volume toward payments for value. In practice, this means introducing incentives for doctors and other health care providers to move from fee-for-service medicine toward payment-for-performance. The best way to accomplish this is an approach called, “bundled payments”, where providers get payment incentives to share risks among everyone necessary to treat patients for that episode of illness. Importantly, bundling payments pays providers for cooperation on coordinated care. The coordination function, enabled by information technology and electronic health records, is especially effective in driving lower costs for the most expensive 10% of patients.
Patients don’t want more medicine, we want more health. This distinction points to a fundamental mismatch of marketplace goals, which reform helps correct.
Brian Gregory, MD, MBA • GAAP versus non-GAAP? EBITDA equivalents for healthcare — but non-financial also? Of course, as in finance you’d need the equivalent of the SEC and auditors to make sure that the standardized reports (books) aren’t cooked.
Maria K Todd MHA PhD • Umm, Scott,
Bundled payments are the primary reimbursement model of medical tourism payments. I think you just made the case why medical tourism might actually be more easily inserted into the mainstream of healthcare reform.
ACA isn’t real until “the Supremes” say it is. Reform, on the other hand…marches on to its own cadence.
Bundled payments are something I’ve been managing for 15+ years. In fact, I’ve managed an integrated group of physicians and ambulatory surgeries that has had bundled payments, case rates and contracts with self funded employers for 15 years – with a track record in payment timeliness and accuracy such that NO payer has been late or paid a claim inaccurately more than 3 times in 15 years since we started.
I can demonstrate first hand, the validity, value-based purchasing, outcomes, and savings of this model probably better than anyone in the country except for those that have worked on this project with me, with a 15+ year track record, and have now overlaid the lessons learned onto MHI’s medical tourism operations…with much success.
What we also see is that the volume of cases tends to improve things like: increased throughput. more cases done by the same team with a team rhythm that enhances case profitability, reduces time under anesthesia, which tends to reduce potential complications of prolonged anesthesia, reduces instrumentation on the field that has to be counted, which takes less time per case, reduces the cost of wasted consumables that have to be billed for on FFS because they were opened, reduces autoclave use, which reduces energy consumption and processing staff, and so on.
Fewer billing and collections staff, one bill, one payment, and settlement to providers that costs us about $0.10 to $0.12 per payment to each physician on the team, all done without human intervention. Am I right Doug?
The limitation is not with the providers, the network, or the ability to contract for bundled payments. The limitation lies with most of the TPAs, ASOs and payers who cannot process bundled payments given their current software systems limitations and their lack of staff to perform these settlements and adjudication manually.
Scott Frankum, MBA • B,
I’m sure you’re right about cooked outcomes…but I don’t think reform makes that easy. A practice or hospital would have to keep two sets of books for outcomes. Insane but not out of the question.
I see outcomes as entirely separate from accounting. The way reform works is that good doctors get a standard reimbursement plus a bonus reimbursement for delivering high numbers in the numerator or, for delivering stable levels at a lower denominator. Bad doctors get the standard minus a penalty for bad numerators or denominators.
Good docs will be twice blessed and bad docs will be twice cursed. You have to remember that docs and hospitals will get value ratings on http://www.HealthCare.gov. Over time, good docs will benefit from higher patient demand and bad docs will see patient flight.
I understand your concern about cooked returns…but remember that the big data….which is what electronic medical records will become…has all kinds of tools at the ready to counteract bad actors. I can imagine that waste, fraud and abuse will show up on lists for further investigation. I’m sure there will be dashboards on the clinic side that show how the practice is doing in comparison and even identify where performance problems are. Big data is a different management world.
I don’t see accounting practice changing. I do see EBITDA improving for smart, innovative medicine.
Maria K Todd MHA PhD • Scott, from the managed care and even Medicare Advantage side of contract language, we have not seen penalties contractually woven into reimbursement formulas for physicians or hospitals except in extremely rare cases. Many of these contracts tend to run through 2014 before the initial term of the agreement can be modified, just so that the payers have providers in their HIE shopping malls.
I have seen cooked returns in the St Louis market where the cooked returns from the payer sampled only 10 claims to determine that a provider charged outside the arbitrarily and capriciously established “market basket” and then eliminated 75% of providers. This action, in turn, forced a cone down of available providers (25% of previous access) which caused backlogs for access, which impeded quality and delayed therapeutic intervention. Who keeps them honest?
Before we rely upon the value ratings on http://www.healthcare.gov, from where does the data come and from which data set and how old is it? How valuable is the value rating?
B. Don’t worry, Scott is on the team, this repartee/banter is all good. Scott and I went part of the way through some of this in Berlin during our tour of the city. We know we have different perspectives. We still admire and respect one another. But neither of us pull punches.
Scott Frankum, MBA • Maria,
I did not make the point well, but totally agree with you. The new challenge for offshore providers will be to meet the new U. S. capabilities in quality measures. U. S. providers will be able to say, “We can do surgery “x” for “y” dollars with “z” outcomes certainty.” Few other countries can match the new measurement capabilities….which to my mind…may become a new sustainable competitive advantage for the U. S.
I bet there will be a lot of interest in your practice and experience as bundled payments mainstream out of pilot programs.
Scott Frankum, MBA • Maria,
I’m a little out of my depth, but let me help where I can.
The law starts out with incentives and loads penalties later on. For example, the incentives for docs to convert to EHR end in 2013 but the penalties don’t kick in until 2015. You probably would not see any contract info on penalties now unless you had a copy of an ACO agreement for the first-adopters. Second adopters chose lower kickers but no penalties.
I’m out of my depth on the policing / security function.
HealthCare.gov, is the main destination for transparency on shopping for insurance, doctors, hospitals, nursing homes, dialysis and home health providers. Hospital ratings, for example, include measures for outcomes, safety and customer service.
There is an overall rating, akin to automobile mileage ratings on new cars. The overall rating unifies representations of many other measures for simple side-by-side comparison. The level of detail at HealthCare.gov will continuously improve and expand. By this I mean that the level of certainty goes up over time. There is some info there now and the big bump will come some time in 2014 because the baselines are being established now.
I perceive a concern with ratings in that few of us want to see masses change doctors for very small differences in quality ratings. So…I think they’re designed to change slowly to discourage moving from a doc with a 9.1 for a 9.3 doc down the road. As for the .gov ratings data….I believe it to be direct from the source. Most of the rating is from how healthy they keep patients, (patient outcomes).
Brian Gregory, MD, MBA • Glad that you two are friends…would hate to be an enemy.
Scott,
Personally, I’ve seen many episodes of suboptimal care misrepresented at M&M conferences. Having been an observer of the incidents, I could appreciate the spin.
I’ve also worked with some anesthesiologists who seemed to keep their names out of the suit database in Florida by pinning it on CRNAs or some other mechanism that I can’t understand.
That’s only my small world, so I suspect that much more is misrepresented in the databases in other departments such as the amputation of the wrong leg in a Florida hospital that was never reported as an incident (they found case when back reviewing following a similar case in the same hospital a few years later.)
Anesthesia charts are notorious for omitting untoward events and short periods of less than optimal vital signs.
I knew a sociopathic general surgeon who wrote over 200 incidence reports for insubordination by nurses. The nurses fortunately were refusing to follow his dangerous or absurd requests. Counting those incident reports would have erroneously indicated terrible nursing care.
Data is always a simple, incomplete projection of reality under the best circumstances. Context and truth require actually being there, or having a surrogate whom you trust.
Scott Frankum, MBA • Brian,
I’m sure you’re right. But, the ACA adds a new check / balance in that Consumers will have access to whatever measures they want to view. I think this means that a segment of customers will keep reporting more honest, because if the reporting does not match the patient’s experience of their own health, patients will become more informed and demanding. It appears that consistently bad actors will have to change or be driven out of practice from lower reimbursements.
There is another dynamic that may help, if has the effects I expect. I assume that data fraud is mostly due to fear of being sued for malpractice. When evidence based treatment becomes more reliably supported by large amounts of data…the environment for defensive medicine will loosen and lighten.
I say this because when doctors have good data, they will be able to say to juries “This is my evidence for diagnosis, which is solid for 95% of patients”. “98% of patients respond well to this treatment and 2% are statistical outliers. The patient suing me is, simply, an outlier. I treated them with the best proven protocols.”
I think that will really change the dynamic and lessen the causes / environment of defensive medicine.
I’m laughing about the way Maria and I must seem to other readers. We share a spirited, information-dense writing style, but I always see the exchanges as an opportunity to learn a lot from her, fast. In my mind, at least, I’m Maria’s biggest fan.
Brian Gregory, MD, MBA • ::grin:: How about ego? In many areas (politics, children, pets, religion, gambling, cars,sports teams,romance, therapies….) people will refuse to accept overwhelming evidence of their incorrect analysis.
Also, in many potentially new therapies and techniques for applying therapies, the kinks need to be worked out before the gains (proven by data analysis) are substantiated. Better theory can take a while to achieve its potential.
Different methods work better and are less risky in different hands. One anesthesiologist will choose general anesthesia when another would choose regional because of differing skill levels with each approach or equipment (iv catheters, intubation approaches and blades, spinal or epidural needles, …)
And, what about different values and risk aversion by patients? DNR orders are an example. Another patient might gamble with her life that antibiotic therapy will save her leg rather than amputate. That’s going to affect specific physician analysis in databases if only the numbers but not the footnotes (charts) are read (which will inevitably happen as with quantity jocks in finance and hedge fund traders).
I’m a big proponent of collecting data. I’m a fanatical proponent of ‘good’ data and expert analysis of that data. My worry is that data (good or bad) will be analyzed / interpreted incorrectly by chance and on purpose. Will the government bodies responsible for this be up to the task? If not, is this an opportunity for smaller, off- shore facilities to achieve better patient results by better data collection and analysis?
Scott Frankum, MBA • Brian,
Have a look here at the PCORI (Patient Centered Outcomes Research Institute), which is a new body under the CMS that was created by reform: http://www.pcori.org/. I’d be very interested to know how you evaluate their capabilities.
To your question about opportunities for smaller facilities, here is what I know. The master data set is maintained by a new department of the CMS. They’ll sell dis-identified data for analysis by researchers (so far I think this is not limited to domestic researchers….international researchers are permitted access).
Data won’t replace the skills or faults of the individual doctor. I always see data framed as “decision support”. Individual doctors won’t be outed for individual mistakes. However, if there is a pattern of bad outcomes, they’ll be punished with lower reimbursements and over-time, have incentives to do the things that make patients healthier.
The next topic was about how quickly new treatments mainstream. The CMS has a new innovation center, http://www.innovations.cms.gov/. And there are “pilot programs” to test good ideas on a larger scale. Accountable Care Organizations are still pilot programs. I think it is helpful to view reform’s changes as an accelerant on learning rather than as a replacement for traditional science.
Last point…I don’t think reform does much about the human condition and cognitive dissonance. If it can, I’ll be the first to sign up for the shots.
Brian Gregory, MD, MBA • Scott,
Ah! We have reached an impass. How do we decide who is has the correct premises? Does it matter?
If I am correct, then one can take advantage of the inability of the government to do an analysis of data it collects. That can lead to relatively better and cheaper healthcare at my facility…hence a potential competitive advantage for an independent off shore facility.
If you are correct, then everyone can use the same analysis with no competitive advantage from it.
This reminds me of sailboat racing. The boat not in the lead will try to sail a different course to take advantage of unforeseen changes in the wind to beat the leading boat. The boat in the lead will tac and jive with the boat behind it to keep that from happening.
Maybe, if I were an off-shore facility, my best course of action (whether or not some US bureaucracies do good, actionable analyses) should be to devise my own system of monitoring the status quo and my improvement initiatives to replace or supplement the ‘generic’ one. Sometimes, the resulting analyses might suggest entirely different ‘courses’ of action.
If I’m correct…and we’re competitors…then I should agree with your premises and hope that you don’t change course.
🙂
Brian Gregory, MD, MBA • In finance an analogy, of sorts, would be a predatory algorithm.
Brian Gregory, MD, MBA • As for new treatments mainstreaming:
The anesthesia literature often lagged how we practiced by a couple of years. In the case of neuroanesthesia, one faction refused to acknowledge they were wrong about patient hydration for a decade before overwhelming data convinced practitioners to ignore them.
Some of the published papers stated what had been considered common knowledge for years, and not a few of them were irrelevant clinically. The statistical analyses done in some premier medical journals has been shown to be of the wrong type or incorrectly applied in 50% of cases (this isn’t taking into account bad data and other types of poor reasoning.
The practitioners who don’t take the literature with a grain of salt are sometimes considered naive. The literature can be good for ideas that are implemented and modified with experience.
So, how will this analyzed data be used? Enforced into practice? Or just as guidelines? Willl it be the basis of lawsuits? Standard of care?
Scott Frankum, MBA • Brian,
I think you’re absolutely right different responses to data. I know first hand that the Cleveland Clinic is selling their internal systems / methods by selling a software package, SAS, to others. Perhaps an analogy is a slow-moving stock market, where different actors act differently on the timing and completeness of the data. I just don’t know enough to speculate much beyond this.
A question, please. If both of us are basically right, do you think the quality of care will get better or worse, overall? Do you see barriers to data becoming constructive or, do you think data will become dystopian?
As you can tell, I’m super-hopeful but also know that things can go wrong.
Brian Gregory, MD, MBA • You’ve taken the optimistic viewpoint,and I the pessimistic
I hope you are right and I’m wrong. If we sat down and discussed this over a couple of good German beers, by the end of the night we would conclude ,without a doubt, that Germans would continue to make good beer into the foreseeable future.
.
Maria K Todd MHA PhD • Guys, I commend you both for a wonderful thread. The deepest I’ve seen in a long time on medical tourism, but can we relate it back to the original question? and please, let us not assume that medical tourism infers international hospitals and offshore competitive opportunities. There’s a huge amount of health travel occurring right here in the USA, where all these data collection and reporting systems are co-located.
Brian Gregory, MD, MBA • Sorry Maria…got on a roll. Sometimes, though, one needs to ask a slightly different question to work toward an answer on the first question.
For instance, I think that your original question, “How will medical tourism insert itself into the mainstream of U.S. healthcare reform?”, might better be phrased,”How will medical tourism change mainstream U.S. healthcare reform?”.
You’ve said that you had to further develop the concept of bundled payments with modifications to existing computer programs and accounting systems to make your view of medical tourism work. How do you know that you haven’t already significantly influenced the current drive for ACOs and bundled payments in the US?
Lets work on this concept of bundled payments for a bit.
In a fee for service system when individual compensation seems to be set by insurance companies, HMOs, or the the government, AND when there are regulations against fee splitting or sharing income among the parties involved, the negotiations for fees between the individual service providers for a particular case are limited. Supposedly, the fees paid to each party are related to the schooling, risk involved, or some other ‘deserved’ amount (not necessarily true, but given lip service at least).
Now, if a bundled payment is made then negotiations between involved parties will have to be allowed (at least I think they will). The ‘deserved’ share of the pie concept might fly out the window. Since there are so many necessary services involved in most cases, any one of which could interfere with completion of the care of the patient, any one of those services could hold the others hostage. A supply and demand scenario (unrelated to education or expense of training) could ensue.
What would be the effects of a significant supply and demand healthcare system? Fewer people willing to spend a fortune in time and money for their healthcare education? Specialists being ousted in favor of generalist who can do anything and everything (like the old fashioned country doctor)? Your existing data collection system will probably need altering. I’m sure that you can come up with a lot more ripples (tidal waves?) from this change.
Thoughts?
Brian Gregory, MD, MBA • Maria,
I just realized that I changed your question. What I meant to say was:
“For instance, I think that your original question, “How will medical tourism insert itself into the mainstream of U.S. healthcare reform?”, might find insight from the question,”How will medical tourism change mainstream U.S. healthcare reform?”.
Input, Scott? Anyone?
Scott Frankum, MBA • Good call. I policy-wonked out and forgot the question. I think reform makes domestic or international travel much more likely, because reform makes value visible. Reform unlocks the power of consumers, who will drive all the value creating changes. of which traveling for health is one. . Over time, reform builds the transparency and tools that transition today’s patients into tomorrow’s value-seeking consumers.
My take on the answer has two parts: apples to apples comparisons and health insurance exchanges, (HIX).
If Value = outcomes ÷ costs captures the right priorities and is the unifying principle of ACA reform….and value is publicly visible on HealthCare.gov….and carriers on the new HIX allow payment to the “away” facility….and consumers have skin-in-the-game for payment, (or are clinically sophisticated enough to want to go to a top provider)….then consumers can start to self-serve value-seeking behavior.
I think the question shifts from “Will I go?” to “How much difference does there need to be in either the numerator or denominator for me to act?”.
HIXs will come in many flavors and the carriers will come in even more. Companies on the HIX will all operate under the new missions to create value, which I think will make stark comparison to legacy carriers. Remember that at least one carrier on each state HIX must be a co-op, non-profit, (which I think has the potential to carry out most of the functions / benefits of single-payer type insurance).
Providers on the HIX cannot be owned by a legacy carrier. They’re all new ventures and may be freed-up from the traditional rules of an insurance market place. I can imagine a blue-ocean strategy provider geared to younger, healthier customers that pumps up what has value to that segment and cuts back on the traditional costs which don’t have much meaning to the segment. Seems made for a domestic and international health travel play to me.
The California HIX aspires to be an Apple-storetype experience. (I know what you’re thinking…but imagine if the in-store or on-phone person is trained to guide new customers toward the providers that are a good fit for purpose). Health travel could have advocates in the market place very soon.
Maria K Todd MHA PhD • Problem with your initial assumptions:
“In a fee for service system when individual compensation seems to be set by insurance companies, HMOs, or the the government,….”
“Set” is a poor choice of terms, because for government payers, it is not set by, but instead limited to a maximum allowable – one can always choose to charge less then or more than, but agrees by contract to “accept” a different amount than that which they charge, by contract.
“AND when there are regulations against fee splitting or sharing income among the parties involved”
Where did you get this idea? That is not how the term “fee splitting” works. One has always been able to bundle the rates for discrete services by different providers. One cannot “fee split” on a single service, for example, an office visit (99213). Sharing income between providers must be done according to a legally permissible formula, of which there are numerous options, each viable without treading anywhere near fee splitting, kickback, self referral, or other practices prohibited by federal and state regulations.
“The negotiations for fees between the individual service providers for a particular case are limited.”
These are limited only by leverage, negotiation skill, and business model and level of formal integration.
“Supposedly, the fees paid to each party are related to the schooling, risk involved, or some other ‘deserved’ amount.”
Nah, they are pure and simple related to negotiation by the parties. I’ve built more than 150 integrated health delivery systems, so I know this from experience.
“… if a bundled payment is made then negotiations between involved parties will have to be allowed (at least I think they will). The ‘deserved’ share of the pie concept might fly out the window. Since there are so many necessary services involved in most cases, any one of which could interfere with completion of the care of the patient, any one of those services could hold the others hostage.”
Nope, sorry. When properly designed, each component supply or service has a value established by the parties, or established by the product developer. Hostage scenario won’t happen if there is more than one supplier of a service unless there is naked price fixing and or collusion, (Antitrust 090), which would be per se illegal. In most cases, there is likely to be more than one supplier from which the supply may be obtained. In the event that there is only one sole supplier, then there may be a case of essential market force, which may lead to leverage being the advantage of the consumer, in the event that, for example, all the anesthesiologists and CRNAs all formed one single company to be the only supplier for the network.
“What would be the effects of a significant supply and demand healthcare system?”
More choice and better competitive value-based purchasing opportunities, as defined by the values of the buyer.
“Specialists being ousted in favor of generalist who can do anything and everything (like the old fashioned country doctor)?”
Probably not, unless the market placed the same value on the generalist.
“Your existing data collection system will probably need altering.”
You are assuming that we haven’t taken these considerations into account. That is a fact also not in evidence. 🙂
Scott Frankum, MBA • Brian,
I’ll add this in support of Maria’s comments.
I understand bundled payments in ACA reform to be a counter-balance to the type of relationships you describe. It is helpful to remember that individual ACO’s combine all the different types of providers at the treatment level-all the providers necessary for a very limited number of treatments. If the provider-partners bundle a payment too low….the practice suffers. If they bundled it too expensively…they’ll get less business. The ACO “owns” the patient. If the patient has complications or gets a hospital-related infection…the ACO pays. The patient / carrier pays the pre-set price and no more. The incentives are aligned to cooperate and drive costs out and pay the ACO for coordination.
A large hospital chain may be referred to as an ACO hospital, but what that actually means is the larger entity is a collective of smaller ACOs organized at the treatment – disease level.
The first movers seem to have confidence that they’ll be able to participate in bonus payments as a kicker for the desired behaviors. There will be a national average for most procedures. ACOs that deliver care for under the average will be eligible to share in up to 70% (?) of what they save Medicare.
Last note….the specialist / generalist dynamic has a place in the Medical Home pilots in regard to primary care. The Medical Home notion gives patients who share a disease the option to go to a Medical Home that specializes in the treatment of whatever they have. Old-age, diabetes, cancer, HIV….whatever. The idea is to put a specialist primary care doc in the place of a generalist doc. The payment changes from a per visit model to a monthly fee that is higher per patient, but cheaper than hospitalization….which Medical Home is hoped to prevent.
Maria K Todd MHA PhD • Scott,
Also, some of the disease management, predictive modeling, and case management, and natural language/EMR big data handling tools we place into play through our Axiom Health Group vertical (for ACOs, IPAs, and PHOs, etc.) are ones we’ve tested and proven through Mercury Health Travel’s “globally integrated health delivery system®”. These tools are some of the most respected and leading edge in the world of EBM and predictive modeling of chronic and acute disease. Nobody in medical “tourism” is currently doing this. This was one of our “Blue Ocean” exploits and it has served us well. We can produce seamless continuity of care for the ACO/medical home integrated with health travel/medical tourism COE referrals or to take advantage of price arbitrage.
That was why I took exception to Brian’s assumption that our data collection system will “need” altering.
Scott Frankum, MBA • Maria,
I can’t wait until you make “apps for that”.
I know you have thought about all this, but you could be the connector piece for global providers that want to produce a comparison to U.S. ratings on HealthCare.gov or the hospital Value-Based Purchasing ratings. Or, you could sell/partner the expertise to new HIX carriers. Or, make consumer facing apps by city, region or treatment. Or, you could sell a more customer friendly, independent rating system to the better providers nationally. Sounds like the hard part, your algorithm and data, are already there.
Maria K Todd MHA PhD • At this point, the apps for that seems a loooong way off. If I had an investor that wanted to go those routes and invest the capital, programming and marketing to sell such a tool, I would entertain the idea and participate. I am content to develop that which is currently on my plate.
Through Axiom, we currently offer the expertise and smaller bite-size license portions of the tools available to startup ACOs that don’t have the numbers to play in the bigger sandboxes, (e.g., those that require 30K to 50K lives just to return their calls and take them seriously). We can even lease them the staff to run it all, including the case management and disease management nurses. Bespoke reports can be designed for their specific purposes by programmers we lease them on an hourly or project basis to build report templates, using database tools like Crystal, etc.
The problem with independent rating systems is that, absent psychometrics, accepted validation, and statistically valid sample sizes, it’s just another rating system in the market. You see how difficult that has been for QHA, Temos, MTQua and others that have gone this route. That takes millions to do properly, without the guarantee of acceptance by the market that it has any value. BIG RISK!
Not only that, but in some cases, a comparison to the USA could make the USA look bad, which for those carrying the unconditional “USA is best” torch, invites trouble. To get granular enough for the rest of us to accept or reject is expensive, time consuming and at such time the data could be validated and reported (2-3 yrs post data captue cutoff) the actual situation at the time of publication could be vastly different in terms of quality and value, up or down.
As for HIEs /HIXs, until the Supremes decide, I am not investing in anything to accommodate them, for now. Everything we do at any MHI vertical has to transcend the politics of ACA, and make sense in the market regardless of which party rules, or the Supreme’s decision of live or die or somewhere in between. To do otherwise is red ocean, potentially a non-starter, or a short-lived patch job, rather than a sustainable solution for true health care payment, access and utilization reform.
Brian Gregory, MD, MBA • Quite an interesting discussion, guys. Definitely outside my normal ballpark.