The necessary clinical experience and scheduling backend to implement these strategies is assumed.
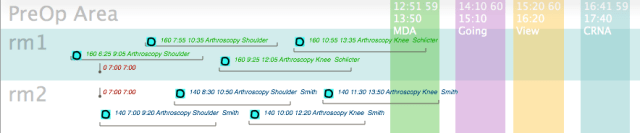
For comparison, two surgeons doing similar cases are used: Dr. Schlicter is flipping between two rooms which for visualization purposes are grouped together into the blue horizontal band labeled ‘rm 1’; Dr. Smith is also flipping between two rooms grouped together in the white horizontal band labeled ‘rm 2′. In subsequent blog posts, the bands will be labeled with the surgeons’ names.
Dr. Schlicter takes 20 minutes longer (surgical+closing time) to do each case. Sometimes he uses a PA (physician’s assistant) to help him start and close (the last 20 minutes) cases.
Dr. Smith is the faster surgeon (20 minutes faster). He also uses a PA–but only to help start his cases.
The first graph represents the difference in time if both surgeons sequentially follow themselves in their own room (block booking). Dr. Smith finishes at 16:20, Dr. Schlicter closes (does not let the PA close alone) and finishes the day at 17:40– 80 minutes after Dr. Smith.
<Click on each graph to enlarge it>
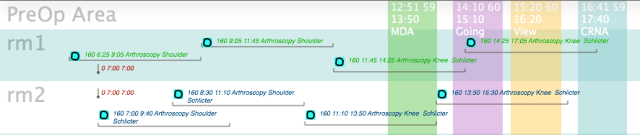
In the following scenario, Dr. Schlicter lets his PA close alone. Notice that there is no change in total OR time compared to Dr. Schlicter closing alone. Dr. Smith finished the day 80 minutes before Dr. Schlicter.
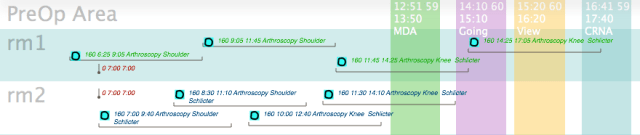
In the following scenario, Dr. Schlicter has his PA help set up each subsequent case so that he (Dr. Schlicter) can immediately go to the next room and cut after closing the current case. Dr Smith is also ‘flipping’ rooms with the aid of his PA. Dr. Smith again finishes the day 80 minutes before Dr. Schlicter, —but both finish 150 minutes early than when not flipping rooms.
In the following scenario, Dr. Schlicter has his PA help set up each subsequent case then come in to close the current case (letting Dr. Schlicter out) so that Dr. Schlicter can be ready to cut when the nurses have finished prepping the subsequent case. [two PAs working in concert would be even better]. Dr Smith is also ‘flipping’ rooms with the aid of his PA. Dr. Schlicter, having saved an additional 6o minutes (saving 210 minutes total), finishes the day only 20 minutes after Dr. Smith.
Below…if Dr. Schlicter wished to say that he finished 4 cases before Dr. Smith, he could arrange to have his ‘cut’ time start at 7:00 instead of room setup starting at that time. An additional saving of 35 minutes has Dr. Schlicter finishing 15 minutes before Dr. Smith!
Continuing with early/on-time starts, the following two graphs compare Dr. Schlicter to himself—showing the comparative advantage of early starts/on-time starts to flipping rooms. The first graph shows the entire day effect of a 7am ‘cut’ time compared to a 7am ‘room setup begins’ time. The end time moves forward by a paltry 35 minutes.
Compare the entire day savings of 35 minutes (above) to the savings of 210 minutes(below) by utilizing the PA in the most efficient manner. Flipping rooms with a PA gets Dr. Schliter out 175 minutes (almost 3 hours) earlier than does an early start with a PA using only one room.
The emphasis is on intelligent scheduling and not having the surgeon (and others) waiting in a non-productive manner.
ORs are rarely fully utilized for more than a few hours a day, and these ‘crunch’ times are often due to the perverse problem that the surgeons are forced to follow themselves in one room and therefore demand an early start time so that they can finish their case load during the working hours that day. If they were allowed to flip rooms, they could start much later (no competition for 7am starts) without the ensuing fights over those time slots.
Those long hours of inactive ORs could be better scheduled, and may even begin to be used with concomitant revenue generation.
There’s no need for additional nursing staff for similar reasons; in fact, overtime may actually decrease.
I used PAs as my example with the knowledge that the orthopedic surgeon would intuitively substitute residents, first assists, scrub techs, and even other surgeons into the argument.
The best mix of any of these resources for a particular surgeon and facility depends on their combined unique scenario. The amount of revenue (or other valuable increment) from the additional free time is quite variable for the surgeon/facility and can be from zero to more than a thousand dollars an hour for each surgeon. The continued competitive advantage of a hospital or outpatient facility has been based on much less than rapid throughput for surgeons.
There’s a lot more that can be done with intra-case optimization dealing with parallel vs sequential tasking, ordering of tasks, and intra-case task placement into specific time slots so as to decrease the specific case duration and also its unrecognized effects on the whole OR schedule and clinicians involved.