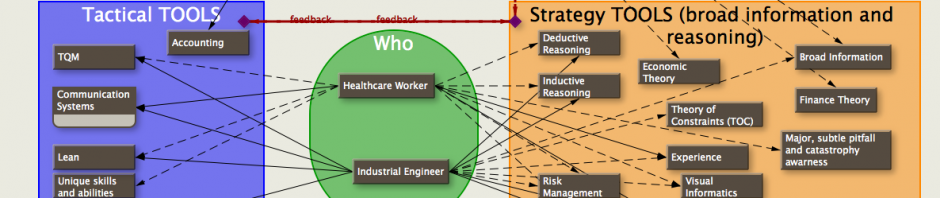
Why is this important?
- It can significantly increase total throughput and throughput as referenced by a particular agent (surgeon, anesthesiologist, hospital).
- Increased throughput can be converted into large increases in revenue.
- It can decrease cost for all agents.
- It can decrease risk.
- It can increase satisfaction for all involved.
More accurate predictions give the PACU staff, OR staff, and Anesthesia staff the ability to anticipate a time slot in the OR schedule. It changes the feeling of frenzy and chaos to one of control and accomplishment. Minor changes before the day starts, or as the day progresses, make a big difference.
Below are some of the charts that go with analysis of a hypothetical OR case schedule. The charts are dynamic (within the software program) and can be used for analysis before, during, or after the cases are actually being done. The data is relevant for algorithm creation depending on policies for PACU, surgeons, anesthesia, OR and PACU expansion and architecture design, etc.; or for just maximizing throughput as changes occur.
The Gantt chart on the bottom right shows 19 cases. Four of the surgeons, each with 4 cases, are running parallel rooms (flipping) to decrease their total time in the OR. There are 3 other surgeons, each who does a single case. It would be an easy matter to decrease the number of rooms by 3 (and concomitant staffing) with simple adjustments to the schedule beforehand, or taking advantage of the normal variance in case length as it manifests. Additional surgeon time would be minimal and the effects on staffing can be seen (more so with additional charts). Cases could also be strategically delayed or expedited to decrease costs.
Top left chart: the number of cases starting in the OR for each time slot.
Bottom left chart: the number of cases ending in the OR for each time slot.
Top right chart: the number of cases starting or ending in the OR for each time slot.
–
click to enlarge

Give Information To Those Who Can Immediately Use It
STRATEGY!
The point of these charts is that different groups can incorporate the same information for their own purposes.
–
The PACU nurses (pre-op side) will incorporate the information to what they already know and decide which patients to send for depending on the distance from the OR, number of orderlies, floor policies, hold time in pre-op area for patients depending on surgeon (always late?) and policies, number of bed slots, number of pre-op nurses and policies for nurse-to-patient ratio, whether to delay sending for patients due to back up through recovery, and adjust factors for same.
–
The PACU nurses (post-op) will know when to give breaks (and to whom), when to set up equipment, when to expedite patients to the floor depending on incoming patients and orderly availabilities, and adjust factors for same.
–
The Anesthesiologists will know how many and when CRNAs and MDAs are needed (adjusting quickly for type of case, surgeon, etc), when to give breaks, more, and how to adjust the flow to accommodate for any constraints. [There are other charts that adjust for all of this automatically.]
–
Surgeons can adjust for available gaps in the schedule, or for planning ahead of time and afterward with regards to PAs, office hours, completing charts, etc.
–
Analysis can be done later for causes of bad ‘clumping’ of surgical starts, best types of surgical cases to schedule at the same time or same day, and of course all the data from the Gantt chart on lengths of cases related to surgeon, procedure, and (with other charts) more details of intra-case events.
–
The floor units can use the data for anticipating sending or receiving patients to or from surgery (this can take 30 minutes or more to organize– sometimes much more depending on medicines, tests, and procedures also scheduled).
–
Similar charts can be adapted for use in the ER.
About Brian D Gregory MD, MBA
Board Certified Anesthesiologist for 30 years. TOC design and implement for 30 years.
MBA from U of Georgia '90: Finance, Data Management, Risk Management.
Practiced in multiple US states and Saudi Arabia at KFSH&RC and KFMC
Taught residents in two locations. Worked with CRNAs for 20 years.