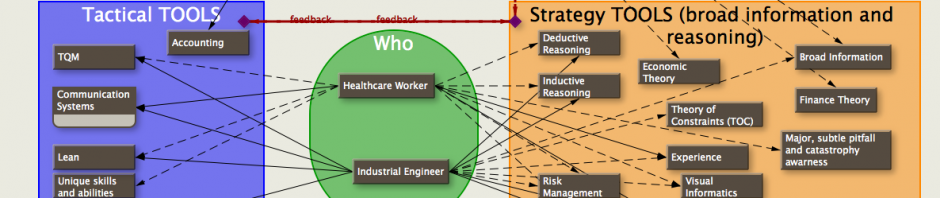
After trying to modify the simulation part of my OR scheduler, and encountering various conundrums, I decided to try to formally clarify the source of the conundrums which led me to other realizations:
To wit:
The important parts of decision making involving processes in a healthcare setting are:
1. Are the results available when they are needed
2. In what context (place and time) can the task be parallel processed (interfere least with other processes)
3. What beneficial or detrimental effects will the process have on other processes?
4. Is the process marginally income efficient.
–
Each of these questions is very context dependent, usually not independent, and can be interpreted only in the FOR (frame of reference) of a particular agent (hospital, physician, insurance company). If you were to try to write a computer program to cover every contingency, you’d have ‘if and else’ stretching from here to the next galaxy.
Clinicians are used to dealing with context and micro-managing processes to optimize risk, time, cost and income. Their failing is in not having sufficient training to broaden their awareness of risks, time, cost, income and 1,2,3,4 above.
–
So, it’s a matter of clinicians being educated to ask the right questions. The right questions asked, and rapid answers to those pertinent questions will improve the necessary and normal micro-management by the clinician to optimize risk, time, cost and income.
–
Statistics:
With regards to statistics, statistical programs are cheap and omnipresent. Also the value (accuracy?) of statistics depends on pertinent and accurate data. Questions that a particular statistic answers has to be phrased with lots of premises and caveats. In clinical care, often the premises (existing situation) is constantly changing, and the value of a statistic has to be in the context of a particular question.
Like the game of 10 questions, an answer for the clinical problem or process can sometimes be answered by different sets of questions. If you can come up with a set of statistics that are sufficient and reliably accurate to answer the 10 questions….then you have a winner. That’s a difficult job to do, and requires a lot of interaction with the clinicians.
So once again, we’re back to the situation in which educating people to ask the right questions is of the utmost importance.
–
Result:
Maybe we should be educating clinicians so they can broaden the use of their clinical acumen to answer process questions they never thought to ask.