The previous blogs were concerned with economic gains for the different parties (surgeon, anesthesia, hospital) by optimizing the relationship each case had with another case (inter-case) — the OR schedule. Each OR is dramatically different, and what works for one won’t work for another. If you don’t have the means of seeing what’s going on, you’ll find it difficult or impossible to achieve your best returns.
In addition to seeing what’s happening between cases (inter-case), attention needs to be paid to what happens during a case (intra-case). This has a dramatic effect on the inter-case schedule. As an extreme example, if every case took only 10 minutes, the OR schedule would be quite short. A opthalmologist doing ECCE & IOLs will have a completely different OR than an orthopod doing hip and knee replacements. Considering just ophthalmologists, some can perform 3 cataract surgeries an hour in one room, or 6 in an hour with flipping rooms, while other ophthalmologists take over an hour for one cataract surgery. Considering orthopods, the surgical approach to replacing a hip, or type and brand of prosthesis, can double the surgical time.
An easy way of comparing and visualizing the effects of techniques, approaches, ancillary help, and individual people will quickly highlight areas that need one’s focus, attention, and possible intervention. If a surgeon repeatedly quickly finishes a facet of a procedure, it’d be worth discovering his technique. If an anesthetist routinely has an unusually short induction time for a procedure, it’d be worth finding out why—either to emulate because it’s a slick technique, or to stop because it’s dangerous. Prolonged times on parts of particular procedures could also be related to post-op complications such as infections. Inter-case scheduling is important, but intra-case analysis can have as much or more profound effect on productivity and risk management.
From the above graph, you would have a good idea of which surgeon has his PA do most of his work, which one does not show up on time to start his case, which room quickly preps the patient for surgery, which anesthetist is on time and does a quick induction. The analysis is limited only by the data you collect.
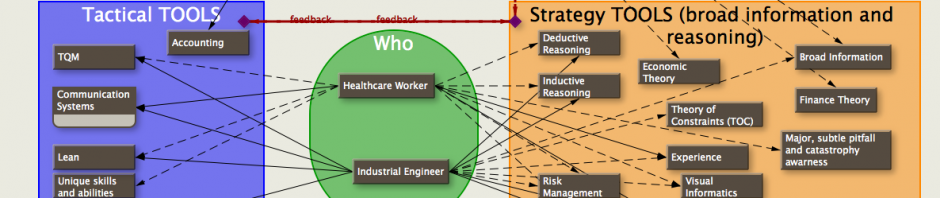

The slope of a segment is correlated with the rate that a particular part of the case is done. One of the axes is time.
The collection of lines (representing time points in individual cases) can be filtered and organized by any combination of procedure, surgeon, room, day of week, etc. The point is to recognize patterns that occur. The causes and deviations of the patterns can be inferred by someone with intimate knowledge of the procedures. Ideally, you could show the graphs to the entire OR crew (surgeons, anesthesiologists, nurses) and let everyone throw in their ideas of what was done particularly well (or not so well) and reasons why the cases deviate from the normal pattern (easily seen and drilled down into). Also, with the ability to quickly filter and organize the graphs–using the right software–larger patterns will emerge that might have to do with something as simple as personnel change during the lunch hour, lack of floor nurses to prep patients, shortage of particular equipment, etc. For example: a scrub tech might know the reason that Dr. Smith’s Total Hip Replacements always take an extra hour on Thursday, a physician assistant might recognize that he/she needs to get to the OR earlier to help organize the positioning of the patient (the OR crew in that room will validate the cause of late starts with that physician assistant), or the delay in starting the next flipped case for that surgeon is due to the large variability in time to close the wound or put on a cast. Lots of causes and interactions, but someone often knows the answers why something works well or doesn’t. The trick is to tap into the collective knowledge of everyone, and the best way to do that is with pattern detection using graphics and some good software. It’s a form of statistical process control with a leaning toward improvement instead of merely status quo.